{ DOWNLOAD AS PDF }
 ABOUT AUTHORS
ABOUT AUTHORS
A.H Ahmed (1), Y.I Alkali (2) U.M Danmusa (3)
1Department of Pharmacognosy and Ethnopharmacy, Faculty of Pharmaceutical Sciences
Usmanu Danfodiyo University, Sokoto- Nigeria
2Department of Pharmacology and Toxicology, Usmanu Danfodiyo University, Sokoto- Nigeria
3Ahmadu Bello University Teaching Hospital Zaria, Kaduna-Nigeria
ABSTRACT
The main aim of this study was to evaluate the prescribing pattern of antibiotics in pediatric patients. A retrospective analysis of patients with bacterial infections admitted into the Paediatric Wards over a period of 3months. Files of 100 patients were randomly selected and included in this study. A proforma was used for data collection, information retrieved from patients records include: Demographic Data, Culture and Sensitivity pattern, Clinical Information, Duration of Hospital Stay, Outcome, type, Class and Route of administration of antibiotics. Out of the 100 patients included in this study, 35(35%) were below one year, 50(50%) were between 1-5years and 15(15%) were between 6-12years. More patients between the ages of 1-5years were admitted with bacterial infections. Out of the 100 patients included in this study 63 (63%) were males and 37(37%) were females. Out of the 100 patients, 27(27%) had septicemia, 48(48%) bronchopneumonia, 6(6%) osteomyelitis, 14(14%) had mixed infections. The remaining patients had urinary tract infection, upper respiratory tract infection and typhoid enteritis. In a total of 229 prescriptions, only 38 (16.6%) were prescribed based on culture result. Most of the antibiotic prescriptions were based on clinical diagnosis, not on culture and sensitivity pattern. In present study 83% of antibiotics were administered by parenteral route and 17% by oral route. The Cephalosporins were the most prescribed antibiotics. Cefuroxime 63(27%) was the most frequently prescribed antibiotic. Ampicillin with Sulbactam was found to be the most frequently prescribed drug combination
Reference Id: PHARMATUTOR-ART-2670
|
PharmaTutor (Print-ISSN: 2394 - 6679; e-ISSN: 2347 - 7881) Volume 7, Issue 07 Received On: 21/05/2019; Accepted On: 05/06/2019; Published On: 01/07/2019 How to cite this article: Ahmed, A., Danmusa, U. and Alkali, yusuf 2019. Prescription Pattern of Antibiotics in Paediatric Wards of a Tertiary Hospital in North West Nigeria: A Retrospective Study. PharmaTutor. 7, 7 (Jul. 2019), 1-6 |
INTRODUCTION
Antibiotics are among the most widely prescribed drugs in Pediatric patients (Choudhury et al., 2013). The world population constitutes of about 28% children and infants, these groups are more vulnerable to bacterial infections due to inadequate immune system (Moorthi et al., 2011).
Antibiotics are prescribed to about 50% to 85% of paediatric patients in developed and developing countries (Paluck et al., 2001). The central role of antibiotics in the treatment of infectious diseases that are prevalent throughout developing countries is undeniable (Palikhe, 2004). However, there are reports of an irrational use of antibiotics which increases the risk of resistance and cost of treatment. Increase in drug resistance and limited availability of newer agents to treat multidrug resistant strains underline the need for rational prescribing (Aparna et al., 2011). Rational use of antibiotic is necessary to avoid multiple drug resistance, treatment failure, non-compliance and increase in cost of therapy (Deshmukh, 2016). Evaluation of drug use in the elderly is a well-researched area, but drug utilization studies in paediatric population are limited (Thapaliya et al., 2015). The main aim of this study is to evaluate the prescribing pattern of antibiotics in pediatric patients.
MATERIALS AND METHODS
1. The Study Area
The study was conducted at the Department of Paediatrics of a Tertiary hospital in North West Nigeria. The Department consists of the Paediatric Medical Ward (PMW), Emergency Paediatric Unit (EPU), the Paediatric Clinic and Special Care Baby Unit (SCBU).
Study Design
A retrospective analysis of patients with bacterial infections admitted into the Paediatric Wards of over a period of 3months
Study Population
Randomly selected files of 100 patients were included in this study
Inclusion Criteria
• Patients admitted with bacterial Infections
• Patients receiving antibiotics
Exclusion Criteria
• Patients with co-morbidities or critically ill
• Patients using antibiotic for prophylaxis purpose
• Patients with Meningitis
2. Data Collection
A proforma was used for data collection, information retrieved from patients records include: Demographic Data, Culture and Sensitivity pattern, Clinical Information, Duration of Hospital Stay, Outcome, type, Class and Route of administration of antibiotics.
3. Statistical Methods
The data obtained was entered into a spread sheet using the Microsoft Excel 2010 and the analysis. Frequency tables and charts were constructed as appropriate. The significance of association between variables was tested using Chi-squared test, where appropriate, for comparison of proportions; while student t-test was used for comparison of means. The level of significance was set at p <0.05.
RESULTS AND DISCUSSION
1. Age Distribution of patients
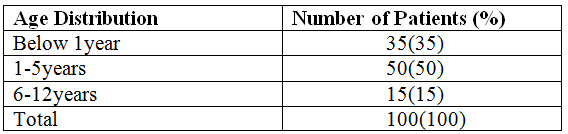
Out of the 100 patients included in this study, 35(35%) were below one year, 50(50%) were between 1-5years and 15(15%) were between 6-12years. More patients between the age of 1-5years were admitted with bacterial infections. This is similar to a study conducted by Dutta et al., 2017 which suggests that children of this age group are more susceptible to infections. Similar results were also reported in other studies (Laya et al., 2015, Kebede et al., 2017)
Table 1 Age Distribution of Patients
2. Sex Distribution
Out of the 100 patients included in this study 63 (63%) were males and 37(37%) were females. Similar results were reported by Thapaliya et al. 2015. According to Muenchhoff and Gaulder 2014, sex has a major impact on outcome from a range of infectious diseases in paediatrics with males having higher morbidity and mortality rates are higher in males than in females which could be attributed to stronger cellular immune response to infection or antigenic stimulation in females than in males.
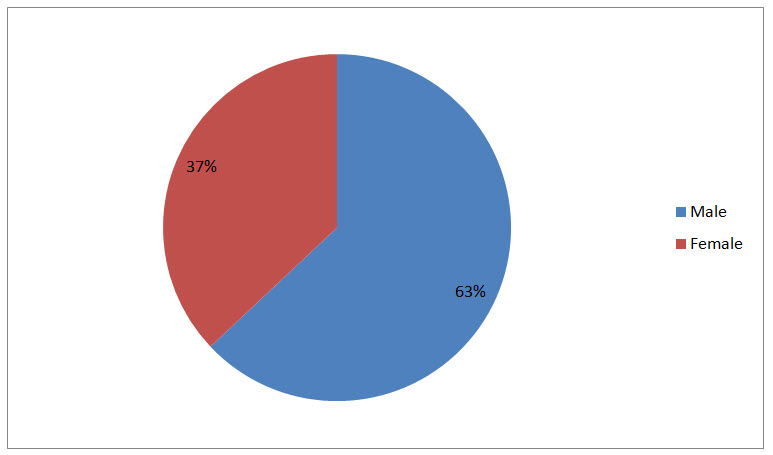
Figure I Gender Distribution of Patients
Pattern of Infection in patients
Out of the 100 patients, 27(27%) had septicemia, 48(48%) bronchopneumonia, 6(6%) osteomyelitis, 14(14%) had mixed infections. The remaining patients had urinary tract infection, upper respiratory tract infection and typhoid enteritis. Bronchopneumonia was the most frequently found infection this is similar to the study reported by Choudhury et al., 2013.
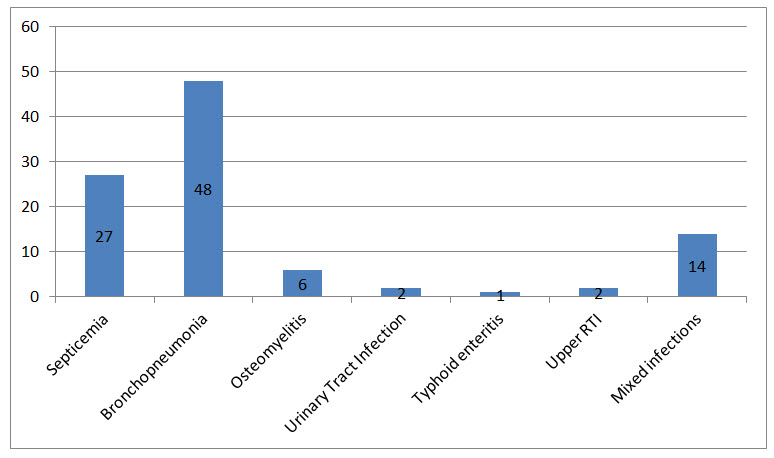
Figure II Pattern of Infection Distribution
4. Culture and Sensitivity Pattern
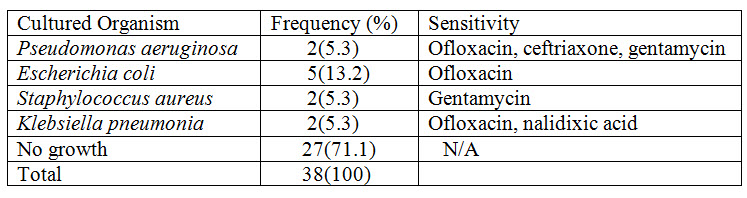
In a total of 229 prescriptions, only 38 (16.6%) were prescribed before culture report. Most of the antibiotic prescriptions were based on clinical diagnosis, not on culture and sensitivity pattern. Culture and sensitivity pattern is important for selection of antibiotics. This will prevent development of antibiotic also decrease the cost of treatment (Leung et al., 2014)
Table 2 Culture and Sensitivity Pattern
5. Route of Drug Administration of Antibiotics
In present study 83% of antibiotics were administered by parenteral route and 17% by oral route. WHO recommends lesser use of parenteral route as it is associated with other problems (Choudhury et al., 2013).
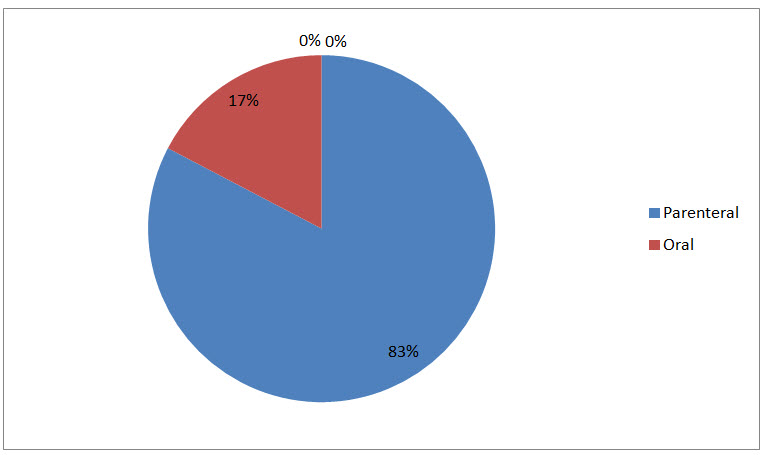
Figure III Route of Drug Administration of Antibiotics
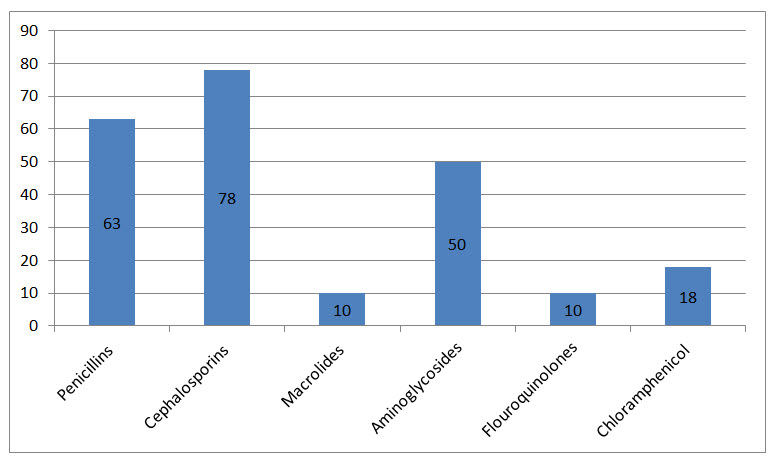
Figure IV Classes of Antibiotics Prescribed
The Cephalosporins were the most prescribed antibiotics which are in agreement with the study conducted by Kanish et al., 2014 which reported that the most common antimicrobial agents prescribed were cephalosporins. Higher prescription rate of cephalosporin may be due to its broad spectrum of activity and tolerance across all age group (Goodman and Gilman 2001).
6. Antibiotics Prescribed
In this study cefuroxime 63(27%) was the most frequently prescribed antibiotic. Ampicillin with Sulbactam was found to be the most frequently prescribed drug combination, this is dissimilar to the study by Sriram et al., 2008 which reported that the amoxicillin with clavulanic acid were the most prescribed. A study conducted by Shamshy et al., 2013 also reported that the most common combination of antibiotics prescribed were Amoxicillin with clavulanate.
Table 3 Antibiotics Prescribed

CONCLUSION
In this study, antibiotic prescription pattern was determined. Most of the antibiotic prescriptions were based on clinical diagnosis, not on culture and sensitivity pattern. Culture and sensitivity pattern is important for selection of antibiotics. Due to increase in antibiotics resistance prescription should be based on culture report.
REFERENCES
1. Choudhury D.K and Bezbaruah B.K (2013); Antibiotic Prescriptions Pattern in Paediatric In-Patient Department Gauhati Medical College and Hospital, Guwahati; J App Pharm Sci, 3 (08);144-148.
2. Deshmukh S. N and Mahajan M. M. (2016) ; A Study of Prescription Pattern of Antibiotics in Paediatric In-Patients at a tertiary care hospital in central India, International Journal of Pharmacological Research; IJPR ; 6(8); 286-289.
3. Dutta S, Bhattacharjee A, Devi M.N (2017); Prescription pattern of antibiotics in paediatric inpatients at a tertiary care hospital in North East India; Int J Basic Clin Pharmacol; 6(10); 2384-7.
4. Goodman & Gilman’s (2001); The Pharmacological basis of Therapeutics; McGraw-Hill Medical Publishing Division; 11th Edition; 1179-1206.
5. Kanish R, Gupta K, Juneja S, Bains H.S, Kaushal S (2014); Prescription pattern of antibiotics in the department of pediatrics in a tertiary care medical college and hospital in northern India; Asian journal of medical sciences; 5(4); 69-72
6. Kebede HK, Gesesew HA, Woldehaimanot TE, Goro KK (2017) ; Antimicrobial use in paediatric patients in a teaching hospital in Ethiopia. Plos ONE; 12(3); e0173290
7. Laya V.R, Modupalli A (2015); Prescribing Pattern of Antibiotics in Pediatric Inpatient Department of a Tertiary Care Teaching Hospital in Bangalore; IOSR Journal of Pharmacy and Biological Sciences (IOSR-JPBS) ; 10(4); 26-32
8. Leung E, Weil E.D, Raviglione M, Nakatani H (2011); The WHO policy package to combat antimicrobial resistance; Bulletin of the WHO 2011; 89; 390-392.
9. Moorthi C, Paul P.R, Srinivasan A, Senthil C.K (2011); Irrational use of antibiotics in paediatric prescriptions: A pilot study at community pharmacy in Erode City; Der Pharmacia Lettre; 3(3); 171-7.
10. Muenchhoff M & Gaulder P (2014); Sex difference in Pediatric Infectious Diseases. The Journal of Infectious Diseases; 209(S3); S120-6.
11. Palikhe, N (2004); Prescribing Pattern of Antibiotics in Paediatric Hospital of Kathmandu Valley. Journal of Nepal Health Research Council; 2(2); 31-6.
12. Paluk E, Katzentein D, Frankish CJ, Herbert CP, Miler R, Speert D et al (2001); Prescription practices and attitudes toward giving children antibiotics; Can Fam Physician; 47; 521-7.
13. Shamshy K, Begum I, Perumal P (2011); Drug utilization of antimicrobial drug in pediatrics population in a Tertiary Care Hospital in Erode, Tamil Nadu, India; International Journal of Pharma Tech Research; 3(3); 1530-1536.
14. Sriram S, Leo M, Manjula Devi A.S, Rajalingam B, Ramkumar K, Rajeswari R (2008); Assessment of Antibiotic Use in Pediatric Patients at a Tertiary care Teaching Hospital; Indian J. Pharm. Pract; 1 (1); 30-6.
15. Thapaliya K, Shakti S, Sheela B, Damodar B, Ram K.C (2015); Prescribing Pattern Of Antibiotics In Pediatric Hospital In Chitwan District In Nepal World Journal Of Pharmacy and Pharmaceutical Sciences; 4(11); 1631-1641
NOW YOU CAN ALSO PUBLISH YOUR ARTICLE ONLINE.
SUBMIT YOUR ARTICLE/PROJECT AT editor-in-chief@pharmatutor.org
Subscribe to Pharmatutor Alerts by Email
FIND OUT MORE ARTICLES AT OUR DATABASE










