{ DOWNLOAD AS PDF }
ABOUT AUHTORS
Debpratim Chakraborty*, Nisha Lama Yolmo
Department of Pharmaceutical tech,
Jadavpur University,
Kolkata, West Bengal, India
*debpratim008@gmail.com
ABSTRACT:
Now a day in medical science and researches, cancer is one of the most life threatening disease but unfortunately still now we have no medical treatment for procurement of this disease. The pathology is not totally clear but according to medical evidence if we consider genes then we must agree that oncogene and tumor suppressor genes are mainly responsible. There are some risk factor also consider which may leads to cancer. The conventional treatments are surgery, Radio-therapy and chemo therapy but the real fact is none of the above mentioned treatment is enough for procurement of cancer and that’s why now scientist and researchers are thinking about nan-technology. NCI has identified that nano-technology have the potential to make paradigm changing impacts on the detection, treatment and prevention of cancer. There are different strategies for cancer therapy using nano-particles like targeted and non-targeted nano-particles. Different studies show that the side effect of doxorubicine (an anticancer drug) can be minimizing by nano-technology, which also reduce the multi drug resistance. Nano-sphere and Nano-capsule of anti-steroid 4-hydroxytamoxifen RU reduce estrogen dependent tumor. Dendritic nano-technology with 5-fluro Uracil decreases the drug clearance and increase the therapeutic time. Methotrixate incorporated dendritic polymer target the folic acid receptor. Camptothecin loaded nano-particles show longer plasma retention, high and longer tumor localization. Nano-particles prepared by poly-lactic-co-glycolide increase the half life of Cisplatin. Paclitaxel, a microtubule-stabilizing agent that promotes polymerization of tubulin causing cell death by disrupting the dynamics necessary for cell division, is effective against a wide spectrum of cancers. Miscellaneous agent like Arsenic trioxide, Butyric Acid, Diethylene-triamine-Acetic acid show more prominent activity. Recent development in nanoparticle-based combination therapy have shown several unique features that are untenable in traditional chemotherapy. Drug combinations can now be optimizedand cleverly delivered in a more effective way.
[adsense:336x280:8701650588]
|
PharmaTutor (Print-ISSN: 2394 - 6679; e-ISSN: 2347 - 7881) Volume 5, Issue 4 Received On: 02/01/2017; Accepted On: 20/01/2017; Published On: 01/04/2017 How to cite this article:Chakraborty D, Yolmo NL;Nano-particles Containing Anticancer Drug; PharmaTutor; 2017; 5(4);12-18 |
REFERENCE ID: PHARMATUTOR-ART-2486
INTRODUCTION:
Cancer is the third leading cause of death (after heart disease and stroke) in developed countries and the second leading cause of death (after heart disease) in the United States. Studies have shown that there were 10 million new cases, 6 million deaths, and 22 million people living with cancer worldwide in the year 2000. These numbers represent an increase of about 22% in incidence and mortality from that of the year 1990. It is projected that the number of new cases of all cancers worldwide will be 12.3 and 15.4 million in the year 2010 and 2020, respectively. In 2008, a total of 1,437,180 new cancer cases and 565,650 cancer deaths were estimated to occur only in the United States [1]. Nanotechnology, an interdisciplinary research field involving chemistry, engineering, biology, and medicine, has great potential for early detection, accurate diagnosis, and personalized treatment of cancer. Nano-particles are typically smaller than several hundred nanometers in size (generally <1000 nm), comparable to large biological molecules such as enzymes, receptors, and antibodies. With the size of about one hundred to ten thousand times smaller than human cells, these nano-particles can offer unprecedented interactions with bio-molecules both on the surface of and inside the cells, which may revolutionize cancer diagnosis and treatment. The most well-studied nano-particles include quantum dot, carbon nano-tubes, paramagnetic nano-particles, liposomes, gold nano-particles, and many others [2].
Pathophysiology: Cancer is fundamentally a disease of failure of regulation of tissue growth. In order for a normal cell to transform into a cancer cell, the genes which regulate cell growth and differentiation must be altered. The affected genes are divided into two broad categories. Oncogenes are genes which promote cell growth and reproduction. Tumor suppressor genes are genes which inhibit cell division and survival. Malignant transformation can occur through the formation of novel oncogenes, the inappropriate over-expression of oncogenes, or by the under-expression or disabling of tumor suppressor genes. Typically changes in many genes are required to transform a normal cell into a cancer cell. Small-scale mutations include point mutations, deletions, and insertions which may occur in the promoter region of a gene and affect its expression or may occur in the gene's coding sequence and alter the function or stability of its protein product. Disruption of a single gene may also result from integration of genomic material from a DNA virus or retrovirus, and resulting in the expression of viral oncogenes in the affected cell and its descendants. Replications of the enormous amount of data contained within the DNA of living cells will probabilistically resulting in some errors (mutations). Complex error correction and prevention is built into the process, and safeguards the cell against cancer. If significant error occurs, the damaged cell can "self-destruct" through programmed cell death, termed apoptosis. If the error control processes fail, then the mutations will survive and be passed along to daughter cell [3].
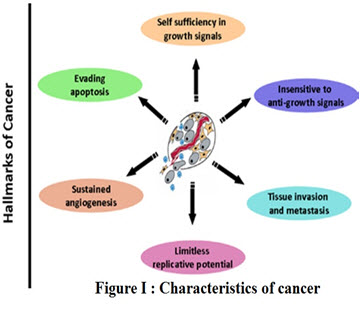
Characteristics of cancer: Six characteristics alterations in cell physiology are associated with malignant growth includes self sufficiency in growth signals, insensitivity to growth-inhibitory signals, evasion of programmed cell death (Apoptosis), (Figure:I) limitless replication potential, sustained angiogenesis, and tissue invasion and metastasis. Each of these physiological changes acquired during tumor development leads to the successful violation of an anti-cancer defense mechanism by the cell and tissues. Six acquired capabilities of cancer. Most of the cancers have acquired these functional capabilities during tumor development [4].
Prevention: Cancer prevention is defined as active measures to decrease the risk of cancer. Thus cancer is considered a largely preventable disease. Risk factors including: tobacco, overweight / obesity, an insufficient diet, physical inactivity, alcohol, sexually transmitted infections, and air pollution [5].
Conventional Treatment Methods
1. Surgery: Surgery, often the first line of treatment for cancer, is used to remove solid tumors (benign tumor as well as in early stage of cancer). But Surgery has no great effect if the tumor is already spread to other organs.
2. Radiation therapy: High energy radiation kills cancer cells by either directly damaging DNA or by generating reactive oxygen species (ROS) preventing cellular division. It is of two forms: a) Brachytherapy- where the radioactive source (in pellets) is placed close to the tumor, eg: uterine cancer and b) Teletherapy- where the patient is irradiated from a source place some distance away from the body. eg, skeletal tumors.
3. Chemotherapy: Chemotherapy is the most widely used therapy method where chemotherapeutic agents (chemicals) are injected or orally delivered to kill rapidly growing malignant cells (Normal cells also killed). Most of these chemicals interfere with normal DNA replication primarily blocking the cells to complete the S phase of cell cycle. In addition there are chemotherapeutic agents cause extensive DNA damage as well as spindle fiber inhibitors [5].
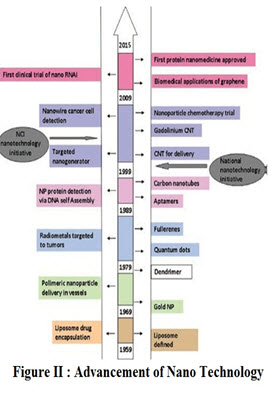
Nano-Particles:
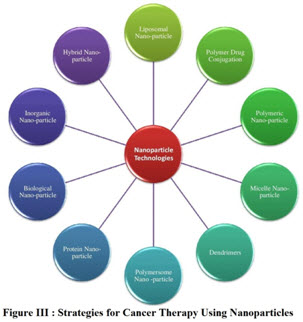
Nano-technology is a multidisciplinary field that uses principles from chemistry, biology, physics, and engineering to design and fabricate Nano scale devices. In its strictest definition, nanotechnology refers to structures with a size range of 1–100 nm in at least one dimension that are developed using top-down or bottom-up engineering. The resulting nano-material demonstrate unique capabilities based on intrinsic properties such as shape and size as well as functional properties conferred through surface modifications as shown in (figure:II) [6] Cancer Institute (NCI) has identified nanotechnology (Figure: III) as having the potential to make paradigm-changing impacts on the detection, treatment, and prevention of cancer.
Strategies for Cancer Therapy Using Nanoparticles: Treatment of cancer therapy acts on three strategies. They are 1. Metastatic Cancer: Spread of cancer cells from the primary tumor site to distant organs, establishing secondary tumor sites is known as metastatic Cancer. Detachment of cancer cells from the primary tumor site and circulation in the blood allows the cells to arrest in organs such as the lungs, liver, lymph nodes, skin, kidneys, brain, colon, and bones, where they can proliferate [7]. Despite significant increases in the understanding of metastatic cancer pathogenesis, early diagnosis, surgical methods, and irradiation treatment, most cancer deaths are due to metastases that are not curable. Reasons for this include resistance to treatments, difficulty accessing the tumor sites and removing all cancer cells during surgery.
NOW YOU CAN ALSO PUBLISH YOUR ARTICLE ONLINE.
SUBMIT YOUR ARTICLE/PROJECT AT editor-in-chief@pharmatutor.org
Subscribe to Pharmatutor Alerts by Email
FIND OUT MORE ARTICLES AT OUR DATABASE
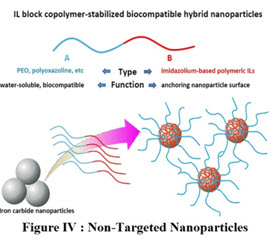
Non-Targeted Nano-particles: Non-targeted nano-particles circulating in the blood have been shown to significantly improve drug bioavailability and accumulation in tumors through the enhanced permeability and retention effect. In general, hydrophobic drugs released extra-cellularly will diffuse and be taken up by cancer cells, leading to enhanced tumor cytotoxicity [8]. Since cancer cell populations, cell density, antigen expression, microenvironment, and vasculature density are significantly different across different cancers and even within primary and secondary metastatic sites, nano-particles bio-distribution and circulation time represent critical parameters for cancer therapy. Multiple factors affect the pharmacokinetic behavior of nano-particles, but the surface charge, size, nano-particle shape and stealth properties are among the most vital (Figure:IV).
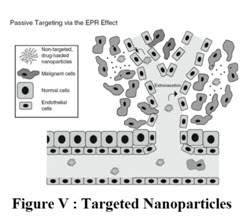
Targeted Nano-particles: The active targeting mechanism takes advantage of highly specific interactions between the targeting ligand and certain tissues or cell surface antigens to increase cellular uptake and increase tumor retention [9]. Conjugation approaches have been developed to control the amount of targeting ligands on the surface of the nano-particles. In the case of weak binding ligands, multivalent functionalization on the surface of the nano-particles provides sufficient avidity. In general, small molecule ligands such as peptides, sugars, and small molecules are more attractive than antibodies due to higher stability, higher purity, ease of production through synthetic routes, and non-immunogenicity. There are two common approaches for receptor-mediated targeting. This first approach is to target the tumor microenvironment, including the extracellular matrix or surface receptors on tumor blood vessel endothelial cells which is usually most efficient for the delivery of immune induction or antiangiogenesis molecules [10]. The second approach is to target tumor cell surfacereceptors for intracellular delivery of cytotoxic agents or signal-pathway inhibitors.(Figure:V)
Anticancer Drug For Nanoparticles
Anthracyclines: One of the most powerful and widely used anticancer drugs is doxorubicin, an anthracyclinic antibiotic that inhibits the synthesis of nucleic acids. This drug has a very narrow therapeutic index as its clinical use is hampered by several undesirable side-effects like cardio-toxicity and myelo-suppression but by nano-technology that side effect may be overcome [11].
Reverse of P-glycoprotein Mediated Multidrug Resistance: Different types of nanoparticles have been developed to reverse the P-glycoprotein mediated multidrug resistance of cancer cells to doxorubicin, an important problem in its clinical use [12].
Antiestrogens: Nanospheres and nanocapsules made of biodegradable copolymers and coatedwith poly(ethylene glycol) (PEG) chains have been developed as parenteral delivery system for the administration of the anti-estrogen 4-hydroxytamoxifen RU 58668(RU). Coating with PEG chains lengthened the anti-estrogen activity of RU, with prolonged antiuterotrophic activity of the encapsulated drug into PEG poly(d,l-lactic acid)nanospheres as compared with non-coated nanospheres. In mice bearingMCF-7 estrogen-dependent tumors, free RU injected by the intravenous route slightly decreased estradiol-promoted tumor growth while RU-loaded PEG-poly- (d,l-lactic acid) nanospheres injected at the same dose strongly reduced it. The antitumoral activity of RU encapsulated within PEGylated nanocapsules wa sstronger than that of RU entrapped with PEG nanospheres loaded at an equivalent dose[13] [14].
Anti-metabolites: Poly(amidoamine) dendritic polymers coated with poly(ethylene glycol) have been developed to deliver 5-fluorouracil. In rats after intravenous administration this nanoparticle formulation showed a lower drug clearance than after the free drug administration [15]. In addition, poly(d,l-lactide)-g-poly(N-isopropyl acrylamide comethacrylicacid) nanoparticles have been studied as drug carrier for intracellular delivery of 5-fluorouracil [16]. Methotrexate has been incorporated in modified poly(amidoamine) dendritic polymers conjugated to folic acid as a targeting agent. These conjugates were injected intravenously into immuno-deficient mice bearing human KB tumors that overexpress the folic acid receptor. Targeting methotrexate increased its antitumor activity and markedly decreased its toxicity, allowing therapeutic responses not possible with the free drug.
Camptothecins: The in vitro and in vivo antitumor characteristics of methoxy poly(ethyleneglycol)-poly(d,l-lactic acid) nanoparticles containing camptothecin have been examined. After intravenous administration in rats, camptothecin-loaded nanoparticles showed a longer plasma retention than camptothecin solution and high and long tumor localization. In both single and double administration to mice bearing sarcoma180 solid tumor, camptothecin-loaded nanoparticles were much more effective than camptothecin solution, in particular the tumor disappeared completely in three of the four mice after double administration of camptothecin-loaded nanoparticles [17].
Cisplatin: Nanoparticles prepared from poly(lactide-co-glycolide) copolymers increase the circulating half-life of cisplatin. A system for the local delivery of chemotherapy to malignant solid tumors has been developed based on calcium phosphate nanoparticles containing cisplatin. Cytotoxicity was investigated in a K8 clonal murin osteosarcoma cell line [18]. Drug activity was retained after adsorption onto the apatite crystals and the apatite-cisplatin formulation exhibited cytotoxic effects with a dose-dependent decrease of cell viability.
Paclitaxel: Paclitaxel, a microtubule-stabilizing agent that promotes polymerization of tubulin causing cell death by disrupting the dynamics necessary for cell division, is effective against a wide spectrum of cancers, including ovarian cancer, breast cancer, small and non-small cell lung cancer, colon cancer, head and neck cancer, multiple myeloma, melanoma and Kaposi’s sarcoma. In clinical practice high incidences of adverse reactions of the drug such as neurotoxicity, myelosuppression and allergic reactions have been reported. Since its clinical administration is hampered by its poor solubility in water, excipients such as Cremophor EL (polyethoxylated castor oil) and ethanol are used in the pharmaceutical drug formulation of the current clinical administration. Mainly active against various brain metastases, though its use in treating brain tumors is limited due to low blood–brain barrier permeability [19].
Miscellaneous Agents:
1. Arsenic Trioxide: Arsenic trioxide was considered as a novel antitumor agent. However, it also showed a severe toxicity effect on normal tissue. To improve its therapeutic efficacy and decrease its toxicity, arsenic trioxide-loaded albuminutes immuno-nanospheres targeted with monoclonal antibody (McAb) BDI-1 have been developed and its specific killing effect against bladder cancer cells (BIU-87) investigated. The albuminutes immuno-nanospheres were tightly junctioned with the BIU-87 cells and specifickilling activity of bladder tumor cells was observed[20].
2. Butyric Acid: Butyric acid, a short-chain fatty acid naturally present in the human colon, regulates cell proliferation. It specifically modulates the expression of oncogenes such as c-myc, c-fos and H-ras, and various genes involved in the activation of apoptosis like p53. The clinical applicability of the sodium salt of butyric acid is limited because of its short half-life of approximately 5 min. To improve its efficacy the pro-drug cholesteryl butyrate has been used as a lipid matrix [21].
3.Cystatins: Cystatins can inhibit the tumor-associated activity of intracellular cysteine proteases-cathepsins B and L and have been suggested as potential anticancer drugs [21].
4.Diethylenetriaminepenta acetic Acid: Since chelating agents exhibit anticancer effects, the cytotoxicity of the extracellular chelator diethylenetriaminepentaacetic acid (DTPA) has been evaluated in breast cancer cell neuroblastoma cells. The anticancer activity of chelating agents is caused by intracellular complexation of metal ions [21].
5.Mitoxantrone:
Mitoxantrone-loaded poly(butyl cyanoacrylate) nano-particles have been tested in leukemia- or melanoma-bearing mice after intravenous injection. Efficacy and toxicity of mitoxantrone nanoparticles were compared with a drug solution and with a mitoxantrone-liposome formulation. The poly(butyl cyanoacrylate) nano-particles and liposomes influenced the efficacy of mitoxantrone in cancer therapy in different ways [22].
NOW YOU CAN ALSO PUBLISH YOUR ARTICLE ONLINE.
SUBMIT YOUR ARTICLE/PROJECT AT editor-in-chief@pharmatutor.org
Subscribe to Pharmatutor Alerts by Email
FIND OUT MORE ARTICLES AT OUR DATABASE
GOLD NANOPARTICLES: Gold nanoparticles(GNPs) are not new; in the 19th century, Michael Faraday published the first scientific paper on GNP synthesis, describing the production of colloidal gold by the reduction of aurochloric acid by phosphorous. In the late 20th century, techniques including transmission electron microscopy (TEM) and atomic force microscopy (AFM) enabled direct imaging of GNPs, and control of properties such as size and surface coating was refined. Common methods of GNP production include citrate reduction of Au [III] derivatives such asaurochloric acid. They have many properties that are attractive for use in cancer therapy. They are small and can penetrate widely throughout the body, preferentially accumulating at tumour sites owing to the EPR effect. Importantly, they can bind many proteins and drugs and can be actively targeted to cancer cells overexpressing cell surface receptors. While they are biocompatible, it is clear that GNP preparations can be toxic in in-vitro and in-vivo systems. GNPs have a high atomic number, which leads to greater absorption of kilovoltage X-rays and provides greater contrast than standard agents. They resonate when exposed to the light of specific energies, producing heat that can be used for tumour-selective photothermal therapy. GNPs have been shown to cause radio sensitisation at kilovoltage and megavoltage photon energies. The exact mechanism remains to be seen but it may be physical, chemical or biological [23].
Future Perspective:
Nanoparticle drug delivery has yielded an unprecedented level of control over the pharmacokinetics of chemotherpeutic agents.
Recent development in nano-particle-based combination therapy have shown several unique features that are untenable in traditional chemotherapy. Drug combinations can now be optimized and cleverly delivered in a more effective way. With a growing alliance between oncologists and engineers, we envision that more therapeutic nano-particles containing multiple drugs with precise drug dosage and release profiles will be developed to treat various types of cancer.
CONCLUSION:
Metastasis is still an extremely complex disease with multiple questions still remaining. While 90% of human cancer deaths are due to cancer metastasis, the hope for fighting cancer is sustained by the fact that there were more than 50 new agents approved in the past 10 years for cancer treatment and hundreds of new agents in clinical development. The development of nano-particle drug delivery systems is expected to have a big impact on the clinical approaches for cancer therapy. The ability to specifically target nano-particles along with the controlled delivery of a therapeutic payload provides powerful new ways to treat cancer which are only starting to be realized. By rationally designing nano-particles based on improved knowledge of cancer biology and the tumor micro-environment, improved efficacy can be achieved. In addition, multi-functional nano-particles able to carry imaging agents and deliver multiple drugs are now being developed for enhanced detection and treatment of cancer. The application of nano-technology to cancer has already produced some exciting results and holds even greater promise for cancer patients in the future.
REFERENCE
1. Journal of the Indian Institute of Science VOL 92:2 Apr.–Jun. 2012
2. Frank Alexis, Eric M. Pridgen, Robert Langer, and Omid C. Farokhzad/ Nanoparticle Technologies for Cancer Therapy,2015
3. Hanan, D., Weinberg, R. A. “Hallmarks of cancer: The next generation”, Cell, 2011 Mar 4;144(5):646-74
4. https://en.wikipedia.org/wiki/Cancer
5. https://en.wikipedia.org/wiki/Management_of_cancer
6. Adler HI, Fisher WD, Cohen A, Hardigree AA (1967) Miniature Escherichia coli cells deficient in DNA. Proc Natl Acad Sci USA 57:321–326
7. James JS (1995a) DOXIL approved by FDA. AIDS Patient Care 9:306
8. Matsumura Y, Hamaguchi T, Ura T, Muro K, Yamada Y, Shimada Y, Shirao K, Okusaka T, Ueno H, Ikeda M, Watanabe N (2004) Phase I clinical trial and pharmacokinetic evaluation of NK911, a micelle-encapsulated doxorubicin. Br J Cancer 91:1775–1781
9. Overall CM, Kleifeld O (2006) Tumour microenvironment - opinion: validating matrix metalloproteinasesas drug targets and anti-targets for cancer therapy. Nat Rev Cancer 6:227–239
10.Salvador-Morales C, Gao W, Ghatalia P, Murshed F, Aizu W, Langer R, Farokhzad OC (2009a) Multifunctional nanoparticles for prostate cancer therapy. Expert Rev Anticancer Ther9:211–221
11. G. Minotti, P. Menna, E. Salvatorelli, G. Cairo, L. Gianni, Anthracyclines: Molecular advances and pharmacological developments in antitumor activity and cardiotoxicity. Pharmacol. Rev. 2004, 56, 185–229.
12. A.C. de Verdie`re, C. Dubernet, F. Ne´mati, E. Soma, M. Appel, J. Ferte´, S. Bernard, F. Puisieux, P. Couvreur, Reversion of multidrug resistance with polyalkylcyanoacrylatenanoparticles: Towards a mechanism of action, Br. J. Cancer 1997, 76, 198– 205
13. T. Ameller, V. Marsaud, P. Legrand, R. Gref, J.M. Renoir, In vitro and in vivo biologic evaluation of long-circulating biodegradable drugcarriers loaded with the pureantiestrogen RU 58668, Int. J. Cancer2003, 106, 446–454.
14.S. Maillard, T. Ameller, J. Gauduchon, A. Gougelet, F. Gouilleux, P. Legrand, V. Marsaud, E. Fattal, B. Sola, J.M. Renoir,Innovative drug delivery nanosystemsimprove the anti-tumor activity in vitro and in vivo of anti-estrogens in human breast cancer and multiple myeloma, J. Steroid Biochem. Mol. Biol. 2005, 94, 111–121.
15.D. Bhadra, S. Bhadra, S. Jain, N.K. Jain, A PEGylated dendritic nanoparticulate carrier of fluorouracil, Int. J. Pharm. 2003, 257, 111–124.
16.C.L. Lo, K.M. Lin, G.H. Hsiue, Preparation and characterization of intelligent core-shell nanoparticles based on poly(D,L-lactide)-g-poly(Nisopropyl acrylamide-co-methacrylicacid), J. Control. Release 2005, 104, 477–488.
17. H. Miura, H. Onishi, M. Sasatsu, Y. Machida, Antitumor characteristics of methoxypolyethylene glycol-poly(DLlactic acid) nanoparticles containing camptothecin, J. Control. Release 2004, 97, 101–113
18. K. Avgoustakis, A. Beletsi, Z. Panagi, P. Klepetsanis, A.G. Karydas, D.S. Ithakissios, PLGAmPEGnanoparticles of cisplatin: In vitro nanoparticle degradation, in vitro drug release and in vivo drug residence in blood properties, J. Control. Release 2002, 79, 123–135.
19. A.K. Singla, A. Garg, D. Aggarwal,Paclitaxel and its formulations, Int.J. Pharm. 2002, 235, 179–192.
20. J. Zhou, F.Q. Zeng, C. Li, Q.S. Tong, X. Gao, S.S. Xie, L.Z. Yu, Preparation of arsenic trioxide-loaded albuminutesimmuno-nanospheresand its specific killing effect on bladder cancer cell in vitro, Chin. Med. J. 2005, 118, 50–55.
21. B. Salomone, R. Ponti, M.R. Gasco, E. Ugazio, P. Quaglino, S. Osella- Abate, M.G. Bernengo, In vitro effects of cholesteryl butyrate solid lipid nanoparticles as a butyric acid pro-drug on melanoma cells: Evaluation of antiproliferative activity and apoptosis induction, Clin. Exp. Metastasis 2001, 18, 663–673.
22.P. Beck, J. Kreuter, R. Reszka, I. Fichtner, Influence of polybutylcyanoacrylate nanoparticles and liposomes on the efficacy and toxicity of the anticancer drugmitoxantrone in murine tumourmodels, J. Microencapsul. 1993, 10, 101–114.
23. S Jain, D G Hirst and J M O’Sullivan, Gold nanoparticles as novel agents for cancer therapy, The British Journal of Radiology, 85 (2012), 101–113.
NOW YOU CAN ALSO PUBLISH YOUR ARTICLE ONLINE.
SUBMIT YOUR ARTICLE/PROJECT AT editor-in-chief@pharmatutor.org
Subscribe to Pharmatutor Alerts by Email
FIND OUT MORE ARTICLES AT OUR DATABASE









