About Author:
Hiren Sakhiya,
M.Sc in Clinical Research Management,
Prist University, Thanjavur,
India
*sakhiyahiren@gmail.com
ABSTRACT
Diabetes a chronic (lifelong) disease marked by high levels of sugar in the blood. Diabetes is a common disease in older age, affecting about one in five individuals. In 2000, according to the World Health Organization, at least 171 million people worldwide suffer from diabetes, or 2.8% of the population. Its incidence is increasing rapidly, and it is estimated that by 2030, this number will almost double. Diabetes is also associated with mortality and significant morbidity, including neurological disability. Diabetes affects both peripheral nervous system and central nervous system. Neuropathy along with retinopathy and nephropathy appears in late stage of diabetes but effect on cognition starts in early stage of diabetes. Although the effects of diabetes on the peripheral nervous system are well established, the effects of diabetes on the central nervous system have been less clear. Several studies have found that diabetes is related to dementia and cognitive function. It is unclear in which stage of diabetes the cognitive decrements become manifest and how they progress over time. Study is conducted to confirm the association of cognitive function with diabetes.
[adsense:336x280:8701650588]
Reference ID: PHARMATUTOR-ART-1306
INTRODUCTION:
Diabetes is a group of metabolic diseases in which a person has high blood sugar, either because the body does not produce enough insulin, or because cells do not respond to the insulin that is produced. This high blood sugar produces the classical symptoms of polyuria(frequent urination), polydipsia(increased thirst) and polyphagia(increased hunger).
There are three main types of diabetes:
Type 1 diabetes: It results from the body's failure to produce insulin, and presently requires the person to inject insulin (Also known as insulin-dependent diabetes mellitus, IDDM for short, and juvenile diabetes).
Type 2 diabetes:It results from insulin resistance, a condition in which cells fail to use insulin properly, sometimes combined with an absolute insulin deficiency. (Formerly referred to as non-insulin-dependent diabetes mellitus, NIDDM for short, and adult-onset diabetes)
Gestational diabetes:is when pregnant women, who have never had diabetes before, have a high blood glucose level during pregnancy. It may precede development of type 2 DM.
Sign and symptoms
The main symptoms of diabetes are polyuria (frequent urination), polydipsia (increased thirst) and polyphagia (increased hunger). Symptoms may develop rapidly (weeks or months) in type 1 diabetes while in type 2 diabetes they usually develop much more slowly and may be subtle or absent.
Prolonged high blood glucose causes glucose absorption that leads to changes in the shape of the lenses of the eyes, resulting in vision changes; sustained sensible glucose control usually returns the lens to its original shape. Blurred vision is a common complaint leading to a diabetes diagnosis; type 1 should always be suspected in cases of rapid vision change, whereas with type 2 change is generally more gradual, but should still be suspected. People (usually with type 1 diabetes) may also present with diabetic ketoacidosis, a rapid, deep breathing known as Kussmaul breathing, nausea, vomiting and abdominal pain, and altered states of consciousness.
A rarer but equally severe possibility is hyperosmolar nonketotic state, which is more common in type 2 diabetes and is mainly the result of dehydration. Often, the patient has been drinking extreme amounts of sugar-containing drinks, leading to a vicious circle in regard to the water loss. A number of skin rashes can occur in diabetes that are collectively known as diabetic dermadromes.
Pathophysiology
Insulin is the important hormone that regulates uptake of glucose from the blood into most cells (primarily muscle and fat cells). Therefore deficiency of insulin or the insensitivity of its receptors plays a main role in all forms of diabetes mellitus. Humans are capable of digesting some carbohydrates, in particular those most common in food; starch, and some disaccharides such as sucrose, are converted within a few hours to simpler forms most notably the monosaccharide glucose, the principal carbohydrate energy source used by the body. The rest are passed on for processing by gut flora largely in the colon. Insulin is released into the blood by beta cells (β-cells), found in the Islets of Langerhans in the pancreas, in response to rising levels of blood glucose, typically after eating. Insulin is used by about two-thirds of the body's cells to absorb glucose from the blood for use as fuel, for conversion to other needed molecules, or for storage. Insulin is also the principal control signal for conversion of glucose to glycogen for internal storage in liver and muscle cells. Lowered glucose levels result both in the reduced release of insulin from the beta cells and in the reverse conversion of glycogen to glucose when glucose levels fall. This is mainly controlled by the hormone glucagon which acts in the opposite manner to insulin. Glucose thus forcibly produced from internal liver cell stores (as glycogen) re-enters the bloodstream; muscle cells lack the necessary export mechanism. Normally liver cells do this when the level of insulin is low (which normally correlates with low levels of blood glucose).
Higher insulin levels increase some anabolic processes such as cell growth and duplication, protein synthesis, and fat storage. Insulin (or its lack) is the principal signal in converting many of the bidirectional processes of metabolism from a catabolic to an anabolic direction, and vice versa. In particular, a low insulin level is the trigger for entering or leaving ketosis (the fat burning metabolic phase).
If the amount of insulin available is insufficient, if cells respond poorly to the effects of insulin (insulin insensitivity or resistance), or if the insulin itself is defective, then glucose will not have its usual effect so that glucose will not be absorbed properly by those body cells that require it nor will it be stored appropriately in the liver and muscles. The net effect is persistent high levels of blood glucose, poor protein synthesis, and other metabolic derangements, such as acidosis.
When the glucose concentration in the blood is raised beyond its renal threshold (about 10 mmol/L, although this may be altered in certain conditions, such as pregnancy), reabsorption of glucose in the proximal renal tubuli is incomplete, and part of the glucose remains in the urine (glycosuria). This increases the osmotic pressure of the urine and inhibits reabsorption of water by the kidney, resulting in increased urine production (polyuria) and increased fluid loss. Lost blood volume will be replaced osmotically from water held in body cells and other body compartments, causing dehydration and increased thirst.
Epidemiology
In 2000, according to the World Health Organization, at least 171 million people worldwide suffer from diabetes, or 2.8% of the population. Its incidence is increasing rapidly, and it is estimated that by 2030, this number will almost double. Diabetes mellitus occurs throughout the world, but is more common (especially type 2) in the more developed countries. The greatest increase in prevalence is, however, expected to occur in Asia and Africa, where most patients will probably be found by 2030. The increase in incidence of diabetes in developing countries follows the trend of urbanization and lifestyle changes, perhaps most importantly a "Western-style" diet. This has suggested an environmental (i.e., dietary) effect, but there is little understanding of the mechanism(s) at present, though there is much speculation, some of it most compellingly presented.
For at least 20 years, diabetes rates in North America have been increasing substantially. In 2010 nearly 26 million people have diabetes in the United States alone, from those 7 million people remain undiagnosed. Another 57 million people are estimated to have pre-diabetes.
The Centers for Disease Control has termed the change an epidemic. The National Diabetes Information Clearinghouseestimates that diabetes costs $132 billion in the United States alone every year. About 5%–10% of diabetes cases in North America are type 1, with the rest being type 2. The fraction of type 1 in other parts of the world differs. Most of this difference is not currently understood. The American Diabetes Association cite the 2003 assessment of the National Center for Chronic Disease Prevention and Health Promotion (Centers for Disease Control and Prevention) that 1 in 3 Americans born after 2000 will develop diabetes in their lifetime.
According to the American Diabetes Association, approximately 18.3% (8.6 million) of Americans age 60 and older have diabetes. Diabetes mellitus prevalence increases with age, and the numbers of older persons with diabetes are expected to grow as the elderly population increases in number. The National Health and Nutrition Examination Survey (NHANES III) demonstrated that, in the population over 65 years old, 18% to 20% have diabetes, with 40% having either diabetes or its precursor form of impaired glucose tolerance.
Indigenous populations in first world countries have a higher prevalence and increasing incidence of diabetes than their corresponding non-indigenous populations. In Australia the age-standardized prevalence of self-reported diabetes in Indigenous Australians is almost 4 times that of non-indigenous Australians. Preventative community health programs such as Sugar Man (diabetes education)are showing some success in tackling this problem.
Currently in the United States 7.8% of the population or around 23.6 million people have diabetes with 5.7 million being undiagnosed. Most of those diagnosed have Type-2 diabetes and are usually 45 years of age or older. But this snapshot is changing as more children and adolescents are increasingly being diagnosed with this type of diabetes.
Studies show that the most common complication of Type-2 diabetes is cardiovascular and it is also the most costly complication at a cost of approximately $7 billion of the $44 billion annual direct medical costs for diabetes. This figure is from 1997 and many estimate that these figures could have doubled by now.
As of 2000 it was estimated that 171 million people globally suffered from diabetes or 2.8% of the population. Type-2 diabetes is the most common type worldwide.
Figures for the year 2007 show that the 5 countries with the largest amount of people diagnosed with diabetes were India (40.9 million), China (38.9 million), US (19.2 million), Russia (9.6 million), and Germany (7.4 million).
Currently, India is the diabetes capital of the world. It is estimated that over 40 million of those with diabetes are currently in India and that by 2025 that number will grow to 70 million. In other words, 1 in every 5 diabetics in the world will live in India. Diabetes is the number one cause of kidney failure, is responsible for 5% of blindness in adults and 1 million limb amputations.
Because of the chronic nature of diabetes, the relentlessness of its complications and the means required to control both diabetes and its complications; this disease is very costly, not only for affected individuals and families but also for the healthcare systems. Studies done in India estimate that for a low income family with an adult having diabetes, as much as 25% of the family's income may need to be devoted to diabetes care.
Stress also seems to be a greater risk factor in India for diabetes. It is important to de-stress according to each one's disposition - for example spending quality time with friends and family, Yoga, breathing exercises, walking, meditation, aerobics and other fitness regimen can ward off diabetes.
Preliminary findings of a recent study in India among school children in the higher socio-economic group in Chennai showed child obesity is growing higher and girls were found to be disproportionately "heavier" than boys.
NOW YOU CAN ALSO PUBLISH YOUR ARTICLE ONLINE.
SUBMIT YOUR ARTICLE/PROJECT AT articles@pharmatutor.org
Subscribe to PharmaTutor Alerts by Email
FIND OUT MORE ARTICLES AT OUR DATABASE
Cognition
It is an intellectual and mental process by which one becomes aware of, perceives, or comprehends ideas. It involves all aspects of perception, thinking, reasoning, and remembering.
Cognitivefunctionrefers to a person’s ability to process thoughts. Cognition primarily refers to things like memory, the ability to learn new information, speech, and reading comprehension. In most healthy individual,s the brain is capable of learning new skills in each of these areas, especially in early childhood, and of developing personal and individual thoughts about the world. Factors such as aging and disease may affect cognitivefunction over time, resulting in issues like memory loss and trouble thinking of the right words while speaking or writing.
Humans are generally equipped with a capacity for cognitivefunction at birth, meaning that each person is capable of learning or remembering a certain amount of information. This is generally measured using tests like the intelligence quotient (IQ) test, although these can be inaccurate at fully measuring a person’s cognitive abilities. Infanthood and early childhood are the periods of time when most people are best able to absorb and use new information, with most children learning new words, concepts, and ways to express oneself on a weekly or even daily basis. Capacity to learn slows down little by little as one gets older, but overall cognitivefunction should not deplete on a large scale in healthy individuals.
Certain diseases and conditions may cause a decline in cognitivefunction. Multiple sclerosis (MS), for example, can eventually cause memory loss, an inability to grasp new concepts or information, and depleted verbal fluency. Not all patients who suffer from the condition will experience these side effects, and most patients will retain the ability to speak as well as their general intellect.
Some research suggests that it is possible to enhance cognitivefunction and prevent a natural decline in memory and thought when caused by normal aging. Doing activities such as word problems, memory problems, and mathematics may “exercise” the brain so that fewer cells die or become inactive over time. This can result in a longer period of high-level cognitivefunction, and even increase cognitive skills in some individuals. Just like any other muscle in the body, the brain needs regular stimulation in order to remain strong.
Any symptoms of decreased cognition should be evaluated by a doctor to rule out any serious conditions. MS, for instance, may initially present itself by subtle changes in cognitivefunction before progressing to more severe symptoms. In most cases, memory loss or the inability to think clearly are caused by simple issues that can be remedied easily. Fatigue or stress, for example, can both result in temporary loss of cognition. The problem generally resolves once the underlying issues have been addressed. Prolonged symptoms or those that worsen with time should always be taken seriously, however, as they could signal either a mental or physical disorder.
AIM
To determine association of cognitive dysfunction with early stage of diabetes by using cognitive test questions battery.
OBJECTIVE
Main objective is to evaluate whether cognition is associated with early stage of diabetes using comparison with normal individual.
METHODOLOGY
LITERATURE REVIEW
Literature search and review was performed before writing the protocol from the Cochrane database and other journals. Firstly the search was related to diabetes, cognition and measurement of cognitive function. Secondly the search for relevant studies on relationship between diabetes and cognitive function and then the search has focused towards the study on association of cognitive function with different stage of diabetes. While searching only one study was found that describe the relationship at early stage of diabetes and it shows significant association at early stage. Other relevant articles have helped in deciding and designing the study and writing the protocol of the study and to decide study rationale.
RATIONALE
Diabetes is widely spread all over the world. It affects both peripheral nervous system and central nervous system. Although the effects of diabetes on the peripheral nervous system are well established, the effects of diabetes on the central nervous system have been less clear. Several studies have found that diabetes is related to dementia and cognitive function. It is unclear in which stage of diabetes the cognitive decrements become manifest and how they progress over time.
Study is conducted to confirm the association of cognitive function with diabetes, And also to determine the effect on cognitive dysfunction at early stage of diabetes and progression over time.
STUDY SITE
This study is carried out at three different sites. These are three diabetic hospitals of Dr. AnantYadav, Dr. P. S. Iyengar and Dr. Vivek Aary at Ahmedabad.
STUDY POPULATION
Patients and normal individual, of any age are included in study but their age may be in between 40-60 years. Both genders are included in study. But total number of patients and normal individual must be same and must be same number for age and gender sub-class.
SELECTION AND ENROLLMENT
Patients are identified by physicians. Then patients are provided information about study in their mother tongue verbally and if they are agreed to participate, they are included in study.
INCLUSION CRITERIA
• Patients diagnosed with diabetes before 1 year to 2 year (1.5 +0.5, where 1.5 year is mean and +0.5 year is standard deviation) that is confirmed by respective physician.
• Each normal individual must be of same gender and same age as of each patient.
• Patients willingly participate in the study.
EXCLUSION CRITERIA
• Patients were excluded if they were known to have a history of
– alcohol or drug abuse
– Psychosis
– personality disorder
– dementia, or emotional, psychological, or neurological disorder, unrelated to diabetes.
• Patients diagnosed with diabetes within1 year or before more than 2 year
• Normal individual not of same subclass of age and gender as of each patient
• Patients don’t wish to participate in the study.
STUDY DESIGN
It is an observational and questionnaire based study. Minimum 35 diabetic patients is included in this study and minimum 35 normal individuals with same age group of patients is included. Patients with one to two years after diagnosis are included in this study. Study just takes 5 to 10 minutes of patient.
Study is questionnaire based and test battery of 13 questions is included in this study. Test battery of questions is prepared by using reference of 3MS exam and MMSE questions. Different score is given to each questions and total score of test battery is 70.
After completion of study test score of patients is compared with that of normal individuals using z-test of significance method.
DATA COLLECTION
Questionnaire is a source of data collection. Test battery of 13 questions is prepared. This questionnaire is prepared using MMSE and 3MS as a reference. Different questions have their individual score for answers given by human subject. Total maximum score of test questionnaire is 70. Test battery is tested and approved by doctors of their sites.
STATISTICAL CONSIDERATION
In this study main outcomes are confirmation of relationship between diabetes and cognitive functions and to determine the effect of diabetes on cognitive function at early stage of diabetes.
Test battery of questions is used to evaluate cognitive functions of patients as well as normal individual. Questions are given score and 70 is the maximum score of test battery.
Normal individual of same age and same sex is also used in this study because patients score is compared with that of normal individual.
Sample size is calculated by using following formula:
N=4 σ2 / L2
Using this formula, the sample size for this study is 35 patients in each group at 5% significant level and 95% confidence interval. It means 35 diabetic patients and 35 normal individual. In this calculation, standard deviation of mean is +6 months and allowable error in diagnosis is +2 months.
Depending upon the data that has been collected and the nature of the same appropriate statistical analyses tests will be applied to test the hypothesis.
Z-test is applied using test score of patients and normal individual to test the significance and whether to reject null hypothesis or not. In this study, null hypothesis claims there is no significance difference in cognition between diabetic patients and normal individuals while alternative hypothesis claims existence of this difference. This method confirms the association and strength of association of cognitive dysfunction and diabetes.
ETHICAL CONSIDERATION
The study will be conducted in accordance with the ICMR, schedule Y, Declaration of Helsinki 1964 and other ethical regulations.
Study protocol, questionnaire and any subsequent modifications will be reviewed and approved by the IRB or scientific committee of institute of clinical research (India). Participation in this study is absolutely voluntary. Participants are informed about the study in their mother tongue verbally. The study related nature, purpose, possible risk and benefit are the adequate information which will be providing by the examiner to the study participant. The information related to the withdrawal from the study at any time will be also given to the study participant. Before signing the consent form the participants are allotted time to read, understand the trial related information. Potential participants are free to ask a doubt related to the study. Patient’s initial is used in all test battery to protect patient’s confidentiality.
NOW YOU CAN ALSO PUBLISH YOUR ARTICLE ONLINE.
SUBMIT YOUR ARTICLE/PROJECT AT articles@pharmatutor.org
Subscribe to PharmaTutor Alerts by Email
FIND OUT MORE ARTICLES AT OUR DATABASE
RESULTS:
This study was completed with 86 participants in which 43 participants were diabetic patients and 43 were normal individuals. 43 patients had diagnosis of diabetes before 1-2 years. These participants were screened through inclusion and exclusion criteria. After successfully enrolment in study, participants were asked the questions using test questions battery to answer or to perform tasks.
DEMOGRAPHIC DATA
1. SEX
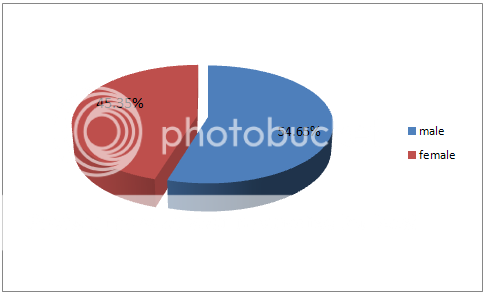
The patient characteristics related to gender (sex) was observed that recruitment of male gender was found to be 54.65% and 45.35% of female. The percentage of the sex ratio of male is much higher than females in the study. This can be seen in the table 1 and fig 1.
Table 1 result of the patient characteristics related to sex
|
Sex |
No. of participants |
Percentage |
|
Male |
47 |
54.65% |
|
Female |
39 |
45.35% |
|
Total |
86 |
100% |
Fig 1 pie-chart of the result of patient characteristics related to sex
2. AGE
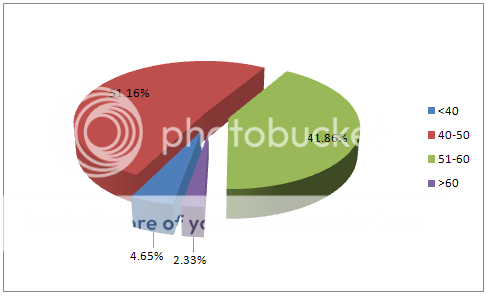
The age group between 40-50 has seen more than 50% involved in this study and lowest percentage of participants are seen from more than 60 years age. This can be easily seen from table 2 and fig 2.
Table 2 result of the patient characteristics related to age
|
AGE (year) |
No. of participants |
Percentage |
|
<40 |
4 |
4.65% |
|
40-50 |
44 |
51.16% |
|
51-60 |
36 |
41.86% |
|
>60 |
2 |
2.33% |
|
Total |
86 |
100% |
Fig 2 pie-chart of the result of patient characteristics related to age
COGNITIVE FUNCTION
In this study, Z-test is performed for the assessment of cognitive function by comparing test score of patients and normal individuals. Results from the calculation of z-test can be seen from table 3.
Table 3 result of cognitive function test questionnaire
|
|
Normal individual |
Diabetic patients |
|
Mean of test score (X) |
67.953488372093 |
67.0930232558139 |
|
∑(x-X)2 |
51.90698 |
47.62791 |
|
Variance |
1.23588 |
1.133998 |
|
Combined SD |
1.088549 |
|
|
SE |
0.234763 |
|
|
Z |
3.665257588713 |
|
|
P one-tail |
0.000123544879767845 |
|
|
P two-tail |
0.00024708975953569 |
|
DISCUSSION:
Diabetes is one of the most common disorders in today’s world. It was observed that insomnia is also affected by many other factors like age factor and education due to less awareness of this disease. Diabetes mainly affects liver, kidney and nervous system and it is its most dangerous effect. It affects both peripheral nervous system and central nervous system. Although the effects of diabetes on the peripheral nervous system are well established and is developed in the late stage of the diabetes but the effects of diabetes on the central nervous system have been less clear. Several studies have found that diabetes is related to dementia and cognitive function. It is unclear in which stage of diabetes the cognitive decrements become manifest and how they progress over time. This study was conducted to establish the relation of diabetes with cognitive functions and to determine the effect on cognitive function at early stage of diabetes. The data of study is collected through test battery. This test battery is consisted of 13 questions. Score is allocated to each question and maximum score of test battery is 70. In this study 43 diabetic patients and same number of normal individuals is included. After successful enrolment of participants in this study, participants were provided information regarding the study and consent was taken from the participants. Then after questions were asked to participants in Gujarati and according to answer score was given to each question for each participant.
From the above obtained data the demographic characteristics in the study shows that the male gender is more affected by diabetes rather than female gender. Through demographic data it can be said through this study at age group between 40-50 age were more found to be diabetic.
This study shows that patients with recent diagnosed type 2 diabetes performed significantly worse on cognitive functions, compared with control subjects. From the data, mean questionnaire score for control participants is 67.95 and for diabetic patients it is 67.09. Variance of questionnaire score for normal individuals is 1.23 and for diabetic participants is 1.13. Z value for these two variance is 3.66 at 95% confidence interval which is higher than 2. Two-tailed P-value is 0.0002 (p<0.05, 95% CI). So, test score of both normal individuals and diabetic patients is highly significant (p<0.05). Test score of normal individuals is significantly higher than that of diabetic patients (one tailed p=0.0001<0.025). Less test score of diabetic patients indicates poor memory function and poor cognitive functions compared to normal individuals.
LIMITATION OF THE STUDY
The major limitation of this study was sample size. Because 43 sample in each group is very small in this type of questionnaire based study. But due to availability of less time and narrow inclusion/exclusion criteria, study was completed with 43 number of participants in each group. This small sample size affects the result and power of the study. If sample size is large in number then the more significant result can be obtain in the results. The tool adapted to collect the data that is test battery that is prepared in reference with MMSE and 3MS. This tool is useful for assessment of only global cognitive function and descriptive measurements. This questionnaire is not useful for assessment of individual cognitive domains like episodic memory, sematic memory, perceptual speed, etc. Though assessment of these domains is possible but due to less time it cannot be performed in this study. It was the major limitation of this study because which domain of cognition is affected due to diabetes cannot be determined.
CONCLUSION
From above over all data analyzed, diabetes affects the central nervous system though exact mechanism is still not known. Diabetes lowers cognitive function and cognitive speed. This effect of diabetes on nervous system manifest in early stage of diabetes though this cannot be said with certainty due to the some limitations of the study, like small sample size, time availability for study, and limited data collection tool. Studies can be performed with higher statistical power and longer duration with new method of data collection to prove the association of cognitive function and diabetes. With higher standard of data collection tools, domains of cognitive functions that can be affected due to diabetes can be determined.
BIBLIOGRAPHY
1. Arvanitakis Z, Li Y, Diabetes Care, 32, 1261-1265 (2009)
2. Arvanitakis Z, Li Y, Diabetes Care, 29, 560-565 (2006)
3. Hu G, Bidel S, Diabetes Care, 30, 842-847 (2007)
4. Folstein MF, Folstein S, McHugh PR: “Mini-mental state”: a practical method for grading the cognitive state of patients for the clinician, Journal of Psychiatric Research , 12, 89-198 (1975)
5. Crum RM, Anthony JC, Bassett SS, Folstein MF: Population-based norms for the Mini-Mental State Examination by age and educational level, Journal of the American Medical Association, 269, 2386-2391 (1993)
6. Tombaugh TN, McDowell I, Psychological Assessment, 8, 48-59 (1996)
7. Yeung SE, Fischer AL, Dixon RA, Neuropsychology, 23, 1-9 (2009)
8. Arvanitakis Z, Wilson RS, Schneider JA, Neurology, 63, 996-1001 (2004)
9. Aggarwal A, Kean E, Neuroscience & Medicine, 1, 39-42 (2010)
10. Cukierman T, Gerstein HC, Williamson JD, Diabetologia, 48, 2460–2469 (2005)
11. Arvanitakis Z, Wilson RS, Bienias JL, Evans DA, Bennett DA, Diabetes mellitus and risk of Alzheimer disease and decline in cognitive function, Arch Neurol, 61, 661-666 (2004)
12. Ott A, Stolk RP, van Harskamp F, Pols HAP, Hofman A, Breteler MMB, Diabetes mellitus and the risk of dementia, Neurology, 53, 1937–1942 (1999)
13. Stewart R, Liolitsa D, Type 2 diabetes mellitus, cognitive impairment and dementia, Diabet Med, 16, 93–112 (1999)
14. Van den Berg E, Kessels RPC, Kappelle LJ, de Haan EHF, Biessels GJ, Type 2 diabetes, cognitive function and dementia, vascular and metabolic determinants, Drugs Today, 42, 741–754 (2006)
15. Manschot SM, Brands AMA, van der Grond J, Kessels RPC, Algra A, Kappelle LJ, Biessels GJ, Brain magnetic resonance imaging correlates of impaired cognition in patients with type 2 diabetes, Diabetes, 55, 1106–1113 (2006)
16. Biessels GJ, Staekenburg S, Brunner E, Brayne C, Scheltens P, Risk of dementia in diabetes mellitus, a systematic review, Lancet Neurol , 5, 64–74 (2006)
17. Manschot SM, Biessels GJ, de Valk H, Algra A, Rutten GEHM, van der Grond J, Kappelle LJ, Metabolic and vascular determinants of impaired cognitive performance and abnormalities on brain magnetic resonance imaging in patients with type 2 diabetes, Diabetologia, 50, 2388–2397 (2007)
18. Awad N, Gagnon M, Messier C, The relationship between impaired glucose tolerance, type 2 diabetes, and cognitive function, J ClinExpNeuropsychol, 26, 1044–1080 (2004)
19. Sandbaek A, Griffin SJ, Rutten G, Davies M, Stolk R, Khunti K, Borch-Johnsen K, Wareham NJ, Lauritzen T, Stepwise screening for diabetes identifies people with high but modifiable coronary heart disease risk, the ADDITION study, Diabetologia, 51, 1127–1134 (2008)
20. Alberti KGMM, Zimmet PZ, Definition, diagnosis and classification of diabetes mellitus and its complications, Part 1, diagnosis and classification of diabetes mellitus, Provisional report of a WHO consultation, Diabet Med, 15, 539–553 (1998)
21. Rutten GEHM, De Grauw WJC, Nijpels G, Goudswaard AN, Uitdewaal PJM, Van der Does FEE, Heine RJ, Van Ballegooie E, Verduijn MM, Bouma M, NHG-standard diabetes mellitus type 2, HuisartsWetenschap, 49, 137–152 (2006)
22. American Diabetes Association, Standards of medical care for patients with diabetes mellitus, Diabetes Care, 25, 213–229
23. Brands AMA, Kessels RPC, Hoogma RPLM, Henselmans JML, van der BeekBoter JW, Kappelle LJ, de Haan EHF, Biessels GJ, Cognitive performance, psychological well-being, and brain magnetic resonance imaging in older patients with type 1 diabetes, Diabetes, 55, 1800–1806 (2006)
24. Graetz P, de Bleser R, Willmes K, AkenseAfasie Test, Lisse, the Netherlands, Swets&Zeitlinger, 1992
25. Schmand B, Lindeboom J, van Harskamp F, Nederlandse Leestestvoor Volwassenen [Dutch Adult Reading Test], Lisse, the Netherlands, Swets&Zeitlinger, 1992
26. Bouma J, Ranchor AV, Sanderman R, van Sonderen E, Het meten van symptomen vandepressie met de CES-D, eenhandleiding, Groningen, the Netherlands, Noordelijk Centrum voorGezondheidsvraagstukken, 1995
27. Van den Berg E, Dekker J, Nijpels G, Kessels RPC, Kappelle LJ, de Haan EHF, Heine RJ, Stehouwer CDA, Biessels GJ, Cognitive functioning in elderly persons
28. with type 2 diabetes and metabolic syndrome, the Hoorn study. Dement GeriatrCognDisord, 26, 261–269 (2008)
29. Lesser R. Verbal and non-verbal memory components in the Token Test, Neuropsychologia, 14, 79-85 (1976)
30. Arvanitakis Z, Wilson RS, Li Y, Aggerwal NT, Bennett DA, Diabetes and function in different cognitive systems in older individuals without dementia, Diabetes Care, 29, 560–565 (2006)
31. Hassing LB, Hofer SM, Nilsson SE, Berg S, Pedersen NL, McClearn G, Johansson B, Comorbid type 2 diabetes mellitus and hypertension exacerbates cognitive decline, evidence from a longitudinal study, Age Ageing, 33, 355–361 (2004)
32. Kloppenborg RP, van den Berg E, Kappelle LJ, Biessels GJ, Diabetes and other vascular factors for dementia: which factor matters most? A systematic review, Eur J Pharmacol, 585, 97–108 (2008)
33. Brands AMA, Biessels GJ, de Haan EHF, Kappelle LJ, Kessels RPC, The effects of type 1 diabetes on cognitive performance, Diabetes Care, 29, 726–735 (2005)
34. Van Harten B, Oosterman J, Muslimovic D, van Loon BJP, Scheltens P, Weinstein HC, Cognitive impairment and MRI correlates in the elderly patients with type 2 diabetes, Age Ageing, 36, 164 –170 (2007)
35. Munshi M, Grande L, Hayes M, Ayres D, Suhl E, Capelson R, Lin S, Milberg W, Weinger K, Cognitive dysfunction is associated with poor diabetes control in older adults, Diabetes Care, 29, 1794-1799 (2006)
NOW YOU CAN ALSO PUBLISH YOUR ARTICLE ONLINE.
SUBMIT YOUR ARTICLE/PROJECT AT articles@pharmatutor.org
Subscribe to PharmaTutor Alerts by Email
FIND OUT MORE ARTICLES AT OUR DATABASE










